Psoriasis
Psoriasis: A Complete Guide to a Chronic Skin Condition
Psoriasis is a chronic (long-lasting) skin condition that is characterized by the formation of red, itchy patches or plaques in the skin. These patches come and go in cycles, flaring for a period of time before subsiding or going into remission. At the moment, there is no cure for psoriasis, and for some individuals, the condition can have a major impact on their life.
Managing the symptoms of psoriasis, including the itch and appearance of the patches, can affect a person’s mental health, work, and relationships. However, while there is no cure presently, there are various effective psoriasis treatments available. It is also possible to incorporate lifestyle changes to make living with psoriasis easier.
Please continue reading to learn more about psoriasis, including why it occurs and how it is treated.
What is psoriasis?
Psoriasis develops when the skin makes new skin cells at an abnormally rapid rate (in days rather than weeks). This causes the skin cells to pile up and form thick, scaly plaques.
What is the main cause of psoriasis?
Psoriasis is an autoimmune disease. It is caused by a problem in the immune system that causes a rapid turnover of skin cells and the formation of psoriatic patches. What causes this immune system malfunction is not entirely clear, but experts believe it is a combination of genetic and environmental factors.
Is psoriasis contagious?
Psoriasis is not a contagious disease. As noted, it is caused by an overactive immune system. Touching or rubbing against a psoriatic plaque will not transfer the disease from person to person.
Who gets psoriasis?
Some 125 million worldwide and 8 million people in the United States have psoriasis. Psoriasis can start at any age but usually begins between the ages of 15 and 35. Men and women are equally affected. However, the prevalence is significantly higher in Caucasians (3.6%) compared to African-Americans (1.9%) – it is possible that psoriasis is under-diagnosed in people of color due to how the patches appear in dark skin (dark brown psoriasis patches in dark skin may not be easily visible).
What are the symptoms of psoriasis?
The most common symptom of psoriasis is the appearance of red plaques covered in thick, silvery scales. A psoriasis plaque can occur as a single patch or join with adjacent patches to cover a large area of skin. Psoriasis plaques are intensely itchy. Some people also experience stinging, burning, pain, or tightness in the affected skin. Other symptoms can include dry, cracked skin that itches or bleeds; thickened, ridged, or pitted nails; and swollen or stiff joints.

Award Winning
We are an award winning dermatology practice that specializes skin.

Experience
Our expert medical providers have years of training and hands-on experience.

Integrated Care
We offer multiple dermatology providers and departments.

Entire Family
We can address dermatology concerns for the entire family at DCA.
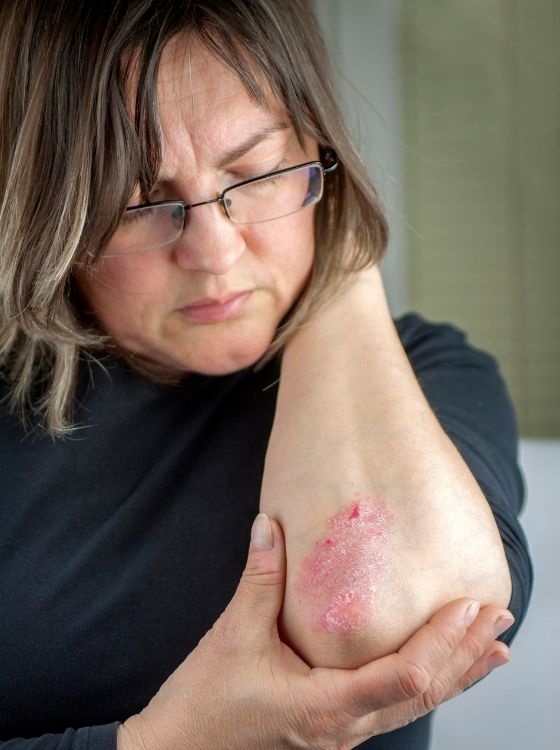
Where do you get psoriasis?
Commonly affected areas include the elbows, knees, lower back, legs, scalp, face, palms of the hands, and soles of the feet.
What are some common psoriasis triggers?
Environmental triggers can cause a flare of psoriasis and start a new bout of the condition. Different people can have different psoriasis triggers, and the triggers can change over time. Some known potential triggers of psoriasis flareups include mental stress; cold, dry weather; heavy alcohol consumption; smoking or exposure to second-hand smoke; injury to the skin such as with cuts, scrapes, insect bites, sunburns, or injections; certain medications, including antimalarial drugs, medications used to treat high blood pressure, and lithium; and infections such as strep throat (the immune system goes into overdrive to fight the infection, starting another psoriasis episode).
Are there different types of psoriasis?
Yes, there are various forms of the disease, including:
Plaque psoriasis: This is the most common type of psoriasis characterized by itchy, tender, red, raised patches covered in silvery scales.
Nail psoriasis: This form of psoriasis causes abnormal growth, pitting, and discoloration of the toenails and fingernails. The affected nail can become loose and separate from the nail bed, and in severe cases, may even crumble.
Inverse psoriasis: This occurs in the folds of skin in the groin, buttocks, and breast and consists of smooth red patches of skin that worsen when the person sweats. This form of psoriasis can be triggered by fungal infections.
Guttate psoriasis: It is triggered by a bacterial infection and tends to occur in children and young adults. It consists of scaling, drop-shaped lesions that usually appear on the arms, legs, and trunk.
Erythrodermic psoriasis: This is a rare form of the disease in which an intensely itchy, burning, peeling, red rash develops, which can cover nearly the entire body.
Pustular psoriasis: It consists of pus-filled psoriatic lesions that often occur in widespread areas of skin or smaller areas such as the palms and soles.
Psoriatic arthritis: This is a type of psoriasis in which the joints become swollen and painful, leading to progressive stiffness and joint damage. Nail changes may also be present.
Does psoriasis have an effect on a person’s general health?
People with psoriasis have a higher risk of developing certain other medical conditions, including psoriatic arthritis, eye conditions such as conjunctivitis and blepharitis, obesity, hypertension, type 2 diabetes, cardiovascular disease, other autoimmune diseases like inflammatory bowel disease (Crohn’s disease), and celiac disease, as well as mental health conditions like anxiety and depression.
How serious is psoriasis? Can psoriasis be life-threatening?
Left untreated, psoriasis can lead to serious medical complications. Erythrodermic psoriasis, a rare form of the disease, can affect nearly the whole body and may be life-threatening.
Will psoriasis go away? Can it clear up on its own?
As mentioned above, psoriasis is not curable at the moment. However, the disease fluctuates, and many people can go without psoriasis flares for years at a time. Proper and timely treatment is essential. Without treatment, psoriasis can lead to severe complications, including psoriatic arthritis resulting in pain, disability, and permanent joint damage.
How is psoriasis diagnosed?
A reputable medical dermatology professional can diagnose psoriasis based on a patient’s history and physical examination. They may take a biopsy (a small sample of skin) for examination under the microscope in a laboratory. This helps to confirm the diagnosis and rule out other similar skin disorders.
How do dermatologists treat psoriasis?
Psoriasis treatment is designed to stop skin cells from growing quickly and relieve symptoms such as itch. Treatment options for psoriasis include topical creams and ointments, oral and injected medications, and phototherapy (light therapy). Here at Dermatology Center of Atlanta, we will work with you and choose treatments based on the type of psoriasis and the severity of the disease, as well as the areas of skin affected. Mild cases can usually be managed with topical creams and ultraviolet light therapy. More severe forms of psoriasis may require systemic treatment to slow down skin cell turnover.
Contact Us
our dermatology
Credentials








