Eczema
Eczema, aka atopic dermatitis, is a common skin condition that can cause your skin to become red and itchy.
Eczema: A Complete Guide to Understanding This Common Skin Condition
Eczema is a skin disorder that causes inflamed, red, itchy, dry, rough, and cracked skin. It affects more than 30 million people in the United States. It is estimated that 1 in 10 individuals in the U.S. will develop eczema during their lifetime. The prevalence of eczema peaks during childhood, but it can occur at any age. Eczema tends to flare periodically and can be accompanied by asthma and allergic rhinitis (hay fever).
Please continue reading to learn more about this skin condition that can have a significant impact on a person’s health and lifestyle. The following paragraphs will describe the causes, symptoms, types, risk factors, complications, prevention, diagnosis, and treatment of eczema.
What causes eczema?
Healthy skin is designed to retain moisture and protect the body against many things such as bacteria, allergens, and irritants. Eczema is caused by a variation in a gene that is responsible for giving the skin its protective qualities. The presence of this gene mutation affects the skin’s ability to provide adequate protection. As a result, the skin is affected by allergens and irritants in the environment.
What are the symptoms of eczema?
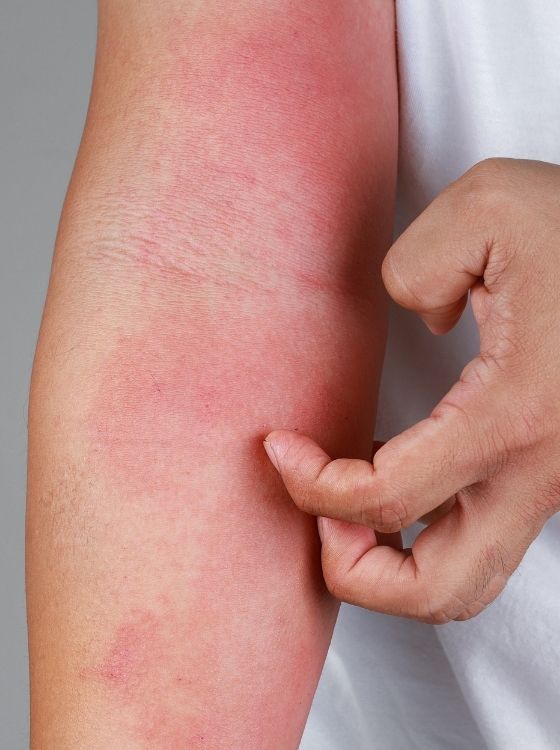
Eczema symptoms can vary depending on the type of eczema and also be different in different people. Common symptoms of eczema include dry skin; itching; red, gray, or brown patches; small raised bumps; thick, scaly, dry, and cracked skin; and/or raw, swollen, or sensitive skin due to scratching.
Who is at risk of developing eczema?
The main risk factor for atopic dermatitis is a personal or family history of eczema, asthma, allergies, or hay fever. The risk factors for other types of eczema can include contact with chemicals or metals, dampness of the hands and feet, mental stress, injuries to the skin, dry skin, and circulation problems in the lower extremities.
What are the different types of eczema?
There are seven different types of eczema:
- Atopic dermatitis: This is the most common form of the disorder. It is caused by variations in genes and is mediated via the immune system. Dry skin and triggers in the environment can make atopic dermatitis worse.
- Contact dermatitis: This type of eczema occurs in response to direct contact with irritants like harsh chemicals or metals. Allergic contact dermatitis is mediated via the immune system and is a reaction to an irritant such as latex.
- Dyshidrotic eczema: A characteristic feature of dyshidrotic eczema is fluid-filled blisters on the hands and feet that itch and hurt. It can be brought on by damp hands and feet, stress, allergies, and exposure to substances like nickel and cobalt.
- Hand eczema: This type of eczema is common in people who work with chemicals that can irritate the skin, such as hairdressers, janitors, dry cleaners, and healthcare workers.
- Neurodermatitis: Thick, scaly patches that are intensely itchy are characteristic of neurodermatitis, which is similar to atopic dermatitis.
- Nummular eczema: This type of eczema consists of round, coin-shaped lesions that are itchy and scaly. The lesions develop in response to an injury such as an insect bite or as an allergic reaction to chemicals or metals.
- Stasis dermatitis: This occurs when weak veins leak fluid, causing the skin to become swollen, red, itchy, and painful.

Experience
Our expert medical providers have years of training and hands-on experience.

Integrated Care
We offer multiple dermatology providers and departments.

Entire Family
We can address dermatology concerns for the entire family at DCA.
Why is it important to treat eczema?
It is important to be evaluated and treated by a medical dermatology professional for eczema. Besides distressing symptoms, untread eczema can lead to complications such as thick, leathery, discolored skin, skin infections due to repeated scratching, and sleep problems due to itching.
How can I prevent eczema?
You can prevent eczema and reduce the frequency of eczema flares by keeping your skin well moisturized. It helps to identify triggers and avoid them as much as possible. Taking short baths and using warm (instead of hot) water can minimize the drying effect of bathing on the skin. It is important to use gentle cleansing agents and skincare products and to dry yourself by patting with a towel instead of rubbing. Lastly, according to the American Academy of Dermatology, people with eczema may benefit from taking a bath with diluted bleach water – this can decrease the number of bacteria in the skin and prevent infections.
How is eczema diagnosed?
There is no specific laboratory test or imaging study to diagnose eczema. Dermatologists make a diagnosis of eczema based on a skin examination and the patient’s symptoms. Sometimes, they may perform a patch test to identify other conditions that may accompany eczema or rule out other skin conditions.
How is eczema treated?
Atopic dermatitis, the most common type of eczema, can be long-lasting and persistent. Most people need to try various treatments before finding one that works for them. Even when treatment is successful, the condition can flare up again, and the signs and symptoms of eczema can return. Early treatment is important, as are self-care steps such as regular moisturizing. Some of the medications used to treat eczema include:
- Corticosteroid creams can help repair the skin and control itching, which is the most common and bothersome symptom of eczema.
- Calcineurin inhibitors such as pimecrolimus (Elidel) and tacrolimus (Protopic) can help control immune system-mediated skin reactions.
- Antibiotic creams may be prescribed to treat secondary bacterial infections as a result of scratching. Antibiotics may also be prescribed to be taken by mouth for a short period.
- Anti-inflammatory drugs (steroids) may be needed to treat severe eczema. However, these medications cannot be used long-term because of serious potential side effects.
- A new injectable biological agent called dupilumab (Dupixent) has been approved by the Food and Drug Administration (FDA) to treat severe eczema. It is a monoclonal antibody that can be effective in people with eczema that has not responded to other treatments.
Are there any non-drug treatments for eczema?
Light therapy or phototherapy, which involves exposing the skin to artificial ultraviolet light, can be effective in treating eczema. However, exposure to UV light can cause premature skin aging and increase the risk of skin cancer.
Another intensive non-drug treatment for eczema is wet dressing therapy, which involves wrapping the affected skin in corticosteroid medication and wet bandages. This treatment, however, is labor-intensive and requires skilled nursing expertise, so it may be offered in a hospital setting to people with widespread eczema.
Counseling can help some people with eczema who are struggling with the emotional fallout of the condition. Relaxation, biofeedback, and behavior modification are other treatment options for eczema that can help reduce habitual scratching.